Understanding the Unusual Case of a Surgeon Who Amputated His Own Legs
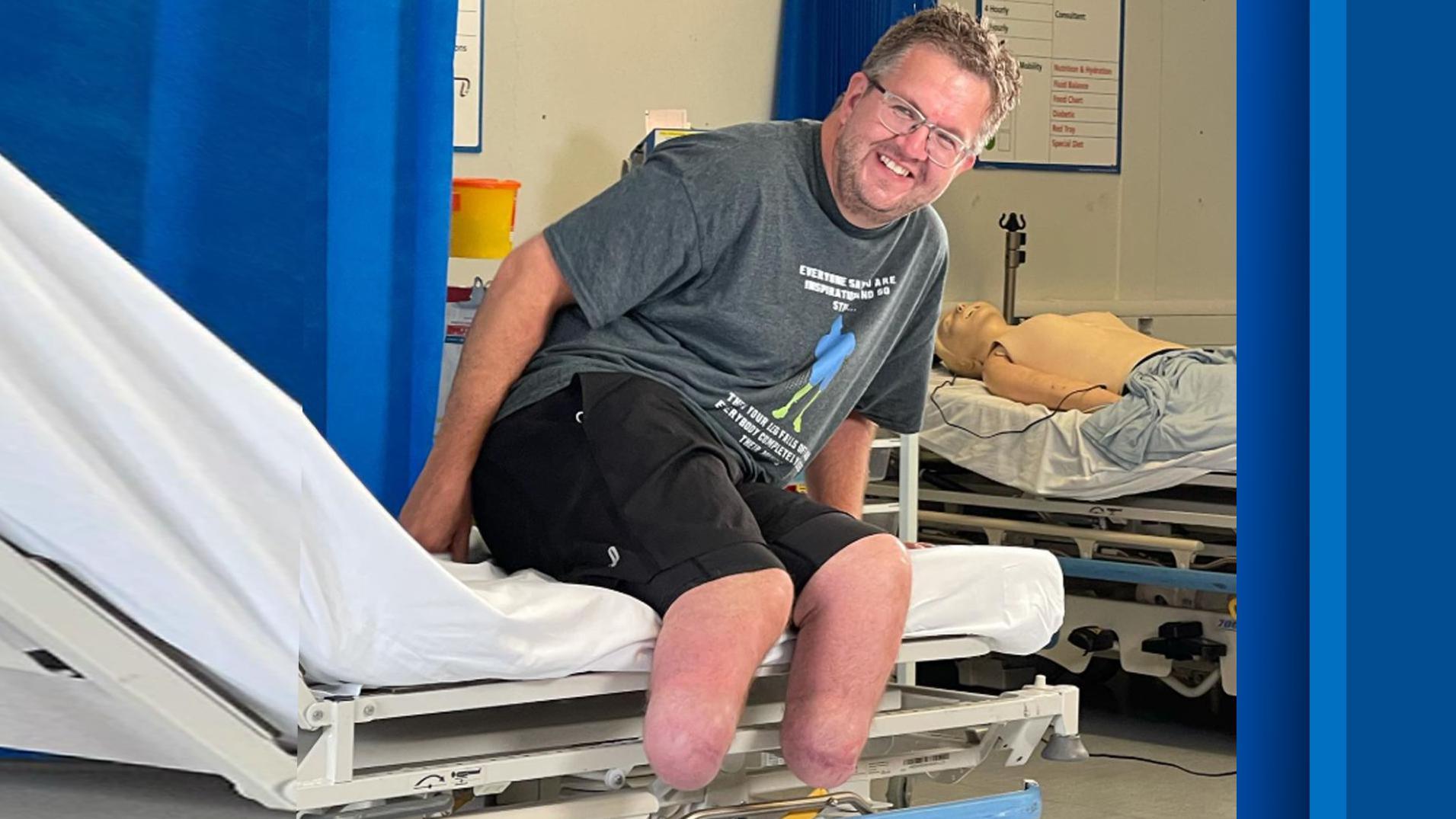
A recent case involving a surgeon who faked sepsis to have his own legs removed has sparked significant debate and raised important questions about mental health conditions. The individual, Neil Hopper, was jailed after pleading guilty to insurance fraud and possessing extreme pornography. It was revealed that he had used dry ice to freeze his legs, forcing their removal in a hospital setting.
Hopper, who grew up in Aberystwyth and Swansea and lived in Truro, Cornwall, had struggled with body dysphoria since childhood. He described his feet as an “unwelcome extra” and a “persisting never-ending discomfort.” Additionally, he had a sexual interest in amputation and had paid for access to videos depicting body mutilation.
This case caught the attention of Dr. Michael First, a professor of Clinical Psychiatry at Columbia University and a research psychiatrist at the New York State Psychiatric Institute. He is known for his work in adding a condition called body integrity dysphoria (BID) to the International Classification of Diseases (ICD), a globally recognized system maintained by the World Health Organization (WHO).
Dr. First first became interested in BID after receiving a phone call from the Muara Digital Team’s Horizon programme. The programme was following the story of two men who would go on to have healthy limbs amputated by a surgeon in Falkirk, Scotland. The hospital trust later banned amputations for psychological reasons.
At the time, Dr. First was working on the Diagnostic and Statistical Manual (DSM), a handbook used by healthcare professionals to classify and diagnose mental disorders. The programme makers were seeking his advice on what mental health condition the men might have. When they called him, he said he had never heard of this condition before, which piqued his curiosity.
Through his early research, Dr. First became aware of conditions such as apotemnophilia and acrotomophilia, where individuals are sexually aroused by the idea of being amputees or have a strong sexual interest in them. He then received a call from a man seeking help, hoping to get a diagnosis that would support his request for surgical amputation.
Dr. First found himself intrigued by the man’s logic. If a condition were listed in a medical manual, it could potentially justify the amputation as treatment. This led him to explore more about the condition.
The Experience of Living with Body Integrity Dysphoria
Dr. First discovered that many individuals with BID felt like they were in the wrong body. They often described feeling like amputees trapped in the bodies of regular people. These individuals, who were otherwise normal, married, and had children, lived with a deep-seated obsession that caused them immense distress.
Many kept their secret hidden, even from their spouses. Dr. First understood why—people might react negatively if they learned about such desires. He noted that these individuals often pretended to be amputees by tying their limbs up or using wheelchairs, which provided some relief.
He observed that the condition typically began in childhood and rarely developed after age 13. Some individuals believed they were born with the condition, while others suggested a triggering event, such as witnessing a classmate become an amputee and gain popularity.
Treatment and Ethical Concerns
Dr. First acknowledged that while antidepressants could help with depression, they did not eliminate the desire for amputation. Antipsychotics showed some success, but the only known treatment that alleviated the mental anguish was amputation itself.
However, this raises ethical concerns. Dr. First expressed fear about the irreversible nature of the procedure. Although he is unaware of any cases where individuals regretted the amputation, those who did may not speak out due to shame.
The condition is believed to be rare, but Dr. First emphasized that many affected individuals remain silent due to stigma. He noted that the condition exists worldwide, yet its true prevalence is unknown.
Conclusion
The case of Neil Hopper highlights the complexities of mental health conditions like BID. While the condition remains poorly understood, it underscores the need for further research and compassionate approaches to treatment. For those affected, support and understanding are crucial in navigating the challenges associated with this unique condition.